This is a quick hypothesis on the need to correct the ability to catabolize retinoic acid (final irreversible product of vitamin A metabolism). This hypothesis is not intended to diagnose, treat, or cure a disease. It is only written for to inform. Please consult with your personal healthcare practitioner before making any changes. I am not a doctor. I am dietitian with a quirky set of skills. – Meredith Arthur, MS, RD, LD
Retinoic acid (RA) has to be catabolized and removed from the body or levels may go to high. Some symptoms that I contribute to high retinoic acid include, nausea, peeling skin, burning sensation of the skin, headaches, fatigue,
This breakdown of RA requires CYP26. There are no known inhibitors of CYP26…yet…but it does require NADPH. This can be made from NAD. In a low NAD state, you won’t have enough NADPH to be able to metabolize retinoic acid. As you work on changing habits that decrease NAD, this NADPH should improve, BUT there is a chance that you are over using all cytochrome P450 enzymes resulting in a burden on NADPH. This could lead to increased levels of RA. High RA can poison a person (think Accutane poisoning). So, I’m working on figuring out how to maximize this NADPH dependent removal of RA.
After it is metabolized by CYP26, the products of RA must go through the glucuronide pathway. There are many substrates that use this pathway. Stevia is one of them. All stevia glycosides are detoxified by this pathway. Monk fruit is also a glycoside, and so uses glucuronidation to be removed from the body. Many drugs use this pathway. So this is another possible inhibitor of properly removing retinoic acid from the body.
There is a vitamin A toxicity group on facebook that has some good information about maximizing these pathways. As I explore this more, I will add what I think is valuable information to this post. So far, these are the most important changes to make to diet (consult your healthcare provider before making changes):
- increase egg yolks to four per day (Andrew Baird from the Vitamin A toxicity group recommends going slow with eggs and starting with one per day https://www.facebook.com/groups/3033243886748451/)
- decrease sweeteners such as monk fruit and stevia
- work on daily bowel movements, but not with Miralax. Magnesium bicarbonate may help as the bicarbonate also triggers mesothelial cells to make acetycholine independent of vagus nerve stimulation. Acetycholine is the major neurotransmitter of the gastrointestinal tract. I used to use Magnesium citrate with Zoey, but just yesterday one of my “treasures in heaven clients”, Meagan, told me she makes magnesium bicarbonate to increase magnesium levels. Well, I said, “You also just helped your GI tract move.” We learned from each other. Life is a team effort and God brings people together for the good of each other.
- consider Taurine supplement to help with bile acid production
- avoid glyphosate as this overloads cytochrome P450 and ties up NADPH in detoxifying it (Go Organic. Avoid non-organic wheat, soy, oats, corn. ) Check out EWG dirty dozen. https://www.ewg.org/foodnews/dirty-dozen.php
- consider supplementation with calcium-D glucurate to support glucuronidation pathway (Thanks, Oskar for piping in on the Vitamin A toxicity group.)
- DO NOT consider inositol to support the pentose phosphate shunt pathway that helps to make NADPH. I will make a post soon on why you should avoid inositol supplements in detail. However, to give a short explanation, inositol can impair the production of cardiolipin by posttranscriptional inhibition of enzymes in this pathway. I believe this production is already impaired by retinaldehyde accumulation that complexes with ethanolamine leading to A2E formation (lipofuscin). This decreases the availability of CDP diacylglycerol which is a precursor for cardiolipin. When cardiolipin levels decrease in the mitochondrial membrane, this can cause oxidative stress and cell death. Having high vitamin A status alone can cause this process by stealing a source of CDP diacylglycerol needed for cardiolipin production, but adding in inositol can completely inhibit this pathway. In fact, A2E accumulation in the eye actually causes damaged to cytochrome C oxidase leading to oxidative stress. Again…longer post coming soon.
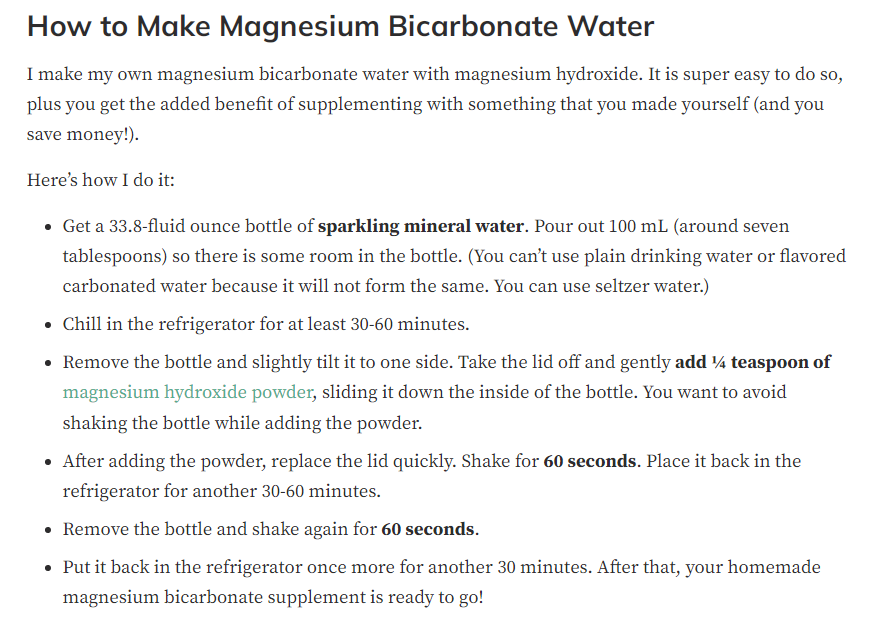
source for MgHCO3 recipe https://wellnessmama.com/health/magnesium-bicarbonate/
Meagan recommends checking on Musclesandmotherhood on instagram for recipes and info about MgHCO3 https://www.instagram.com/_musclesandmotherhood/
This post was reviewed by Jenny Jones, PhD, human molecular genetics. I want to make sure that whatever I share with you has at least two critically thinking minds working on a problem. <3

Thank you so much for these articles, Meredith, and for all the work you (and Jenny) have put into them! 😀 I have been reading them over the past few days, since learning of your blog from Andrew Baird on Grant Genereux’s forum.
I have had debilitating CFS/ME/POTS since I was a teen, and have been on a low-vitamin A diet (under 5% of the RDA) since 2018, which in my case reversed obesity and PCOS (without exercise or caloric restriction—both of which weren’t appropriate for my state of health at that time). However, I started taking inositol around the same time… And whenever I’d stop the inositol, I would get horrible night sweats (so bad they interfered with sleep—I’d wake up drenched in the early hours of the morning).
I’m not nearly to the age of menopause yet or anything. A friend of mine (also younger than menopause age) who limits vitamin A has also found inositol useful for preventing night sweats.
In my case, the night sweats are always much worse in wintertime. It’s summer now, where I live, so I will stop the inositol. If I have worsened my CFS/ME by using it, that’s unfortunate… (But not sleeping worsened it, too, y’know? xD) Anyway, I will be looking forward to your post on that supplement! And if you have an explanation for this night sweat thing, I’d be so curious! 🙂 Part of me always wondered if the solution was to sweat more, but in my condition it would’ve been terribly draining (might be still).
Since I was in my teens, I have had chromhidrosis. My clothes and bedding and pillows would turn a pale rusty orange-yellow. In the last couple of years, this has fortunately lessened dramatically! 🙂
Thanks again for your blog and this post!
You are so very welcome! I hope to keep researching just to help people out.
The night sweat thing is very interesting, and I will look into that, but I have a hypothesis for you because it seems counterintuitive that inositol would help with hypoglycemic induced night sweats as it actually lowers glucose level…so this is a fun puzzle to solve! So it isn’t working that way at all. Perhaps it has to do with acetylcholine levels. When acetylcholine levels are low, the autonomic nervous system can’t work (think of your POTS – and by the way…I have this, but much improved here lately.) Acetylcholine is a muscarinic receptor agonist. I have found that when my acetylcholine is low, I sweat constantly. Do you know what? Restoring my ability to make acetylcholine, and avoiding muscarinic receptor agonist such as monk fruit and stevia has completely changed this. Stevia was giving me unregulated sources of “acetylcholine like” stevia glycosides and so my sweating issue was insane. In any case, I think inositol stops the metabolism of choline sources when levels increase. This makes choline goes up, then you can use it to make acetylcholine! When you have enough acetylcholine the dysfunctional autonomic nervous system that we both have in common because more efficient.
I think the night sweats are because you have something that is impairing your ability to either make or use acetylcholine. Blockers of using acetylcholine would definitely include agonists such as stevia (and I think monk fruit because it causes the same problem for me). Vitamin A toxicity alone will steal your choline away. And…thiamine deficiency will slow down you ability to make acetyl part of acetylcholine. This may be wear inositol helps as well because it pushes you into glycolysis which increases pyruvate, and then perhaps you make more acetyl coA when taking inositol.
So, I think the original sweating back in your teens was a symptom of acetylcholine deficiency due to vitamin A stealing your choline away (ethanolamine retinal steal). Then, your symptoms now are due to being dependent on inositol to help you NOT use choline in your body. This is not good because this, I believe is causing mitochondria to dysfunction….
I believe that inositol can alter cardiolipin production. Cardiolipin can be thought of as a phospholipid that helps with stabilized the mitochondrial membrane. I hypothesize that inositol can turn off the ability to make cardiolipin. This can destabilize super complexes in the mitochondrial membrane leading to inefficient respiratory chain shuttling of electrons towards ATP production. This increases the AMP to ATP ratio. I believe this is how inositol improves glycemic control. It makes it so the same must use glycolysis to generate a small amount of ATP. This is also, in part, how metformin works. Metformin and Inositol are comparable in their ability to promote glycemic control after three months of use. Metformin impairs respiratory complex 1 which has the same effect on the mitochondrial respiration. It increased AMP levels which forces the sell to push more glucose through glycolysis. In addition, if you still have a pretty high total vitamin A level, your cardiolipin production is already impaired by retinal-ethanolamine steal.
If this doesn’t make sense, hopefully the post I am writing will. Let me know if you have questions.
Things that helped me get out of the constant sweats…
1. Thiamine
2. Increased choline intake (eggs)
3. No stevia or monk fruit
4. Sips of baking soda water (helps mesothelial cells that are throughout the body to make and release acetylcholine due to bicarbonate triggers this production)
Of course, I don’t know your entire health history and supplements, so definitely self advocate and talk with your trusted health profession. I’m just one person with a piece of the puzzle. It takes many minds to solve our way out of health issues. Hugs…feeling bad all the time is a downer! I’m so glad you have recovered from PCOS and obesity because that is proof you are on the right track, even if the train is running slowly.